Report: A.LISON, M.GRUENE (GERMANY)
Back to life
A prevention programme for personnel injured in the line of duty − a lifetime concept
In the form of its 'Continuous, interdisciplinary medical care of soldiers injured in the line of duty to restore, retain and improve their psychological and physical capacity' concept, the medical services of the Bundeswehr (German Armed Forces) have evolved a comprehensive medical programme designed for the support of personnel who have been wounded, fallen ill or suffered an accident in the field. This disability prevention programme being implemented in the Bundeswehr's Centre of Sports Medicine is an important element of the 'life-long rehabilitation' strategy.
Introduction
The concept takes as its starting point the definition of disability and the extensive rehabilitation concepts set out in the Convention on the Rights of Persons with Disabilities adopted by the UN in 2006 and ratified by the German Bundestag in 2009. The convention specifies that "persons with disabilities include those who have long-term physical, mental, intellectual or sensory impairments which in interaction with various barriers may hinder their full and effective participation in society on an equal basis with others." The convention goes on to specify in Article 25 that among the health services to which disabled persons are entitled are "early identification and intervention as appropriate, and services designed to minimize and prevent further disabilities [...]." Also stipulated in Article 26 are the provision of "comprehensive habilitation and rehabilitation services and programmes, particularly in the areas of health, employment, education and social services, in such a way that these services and programmes [...] begin at the earliest possible stage, and are based on the multidisciplinary assessment of individual needs and strengths [...]." Rehabilitation thus includes the coordinated use of medical, social, vocational, educational and technical measures and instruments to influence the physical and social environment in order to improve the functioning of disabled persons and thus maintain their maximum independence so that they can participate as extensively as possible in all aspects of life and select their lifestyle as freely as possible.
 The results of performance and functional diagnostic examinations that comply with the
quality standards employed in top-level sports provide the basis for the planning of long term
therapy targets.
The results of performance and functional diagnostic examinations that comply with the
quality standards employed in top-level sports provide the basis for the planning of long term
therapy targets.
Military personnel are at increased risk of suffering some form of damage to their health while in the field. This includes illnesses and traumatic injury that can be either physical (wounds, accidents) or psychological (psychotrauma). Military personnel are completely healthy before they suffer an injury or wound. If their exposure to wounding or the death of comrades in combat results in stress it will usually be a result not only of physical injury but severe mental trauma as well. Due to the high demands many soldiers place on themselves with regard to performance and physical capacity, such a loss of abilities and health has an extensive impact on them. Severe mental traumatic disturbance can in many instances lead to drug problems and/or physical symptoms as a result of inactivity that can take the form of deterioration of efficiency or even internal disorders and pain syndromes in extreme cases. When the body image becomes disrupted in this way, the individual in question requires long term multimodal therapy. The physical resilience of disabled persons can also be extensively reduced by pre-existing and accompanying disorders. Elderly disabled persons, for example, are less capable of adaptation (i.e. do not respond as readily to training) as younger individuals with disabilities or injuries. And persistent physical disabilities are not only a source of major psychological stress for the disabled persons themselves, but also for their families. Hence, nearly all cases of permanent injury sustained in the line of duty require an appropriately designed, multidisciplinary programme of medical care focussing on individual needs, including also family members as far as possible.
Rehabilitation: medical and social case management
The primary aim of a centrally managed programme for continuous aftercare is thus to re-integrate the disabled person in the armed forces and their social environment as rapidly as possible. The German law that sets out the rights of personnel to continue in active duty (EinsatzWVG) specifies that those who have suffered a degree of disability of more than 30% as a result of deployment are entitled to remain in the Bw at their own request. In addition to a moral obligation towards disabled personnel, the Bw also has an active interest in using all means at its disposal to ensure that the physical capacity and abilities and psychological resilience of those affected are restored as far as is possible. The bio-psychosocial model for rehabilitation requires that the work environment in the Bw must conform to the existing abilities of the individual and that those affected must be provided with life-long specialised support in the form of planning and provision of rehabilitation measures, medication and aids, the design of their workplace and the planning of their future vocational activities. Medical and social case management are inseparable elements of this concept and require the continuous exchange of medico-legal and (appropriately protected) confidential information between the two sides.
The medical case manager with appropriate specialist knowledge will be able to make an initial assessment of the subsequent employability of the individual. Sports medicine can contribute orthopaedics, accident surgery, rehabilitation, performance diagnostics and preventive medical expertise, sports therapy and its physical and psychological training techniques; however, educational and social elements can also make an important contribution towards restoring the psychophysical resilience of the injured individual and thus help with their reintegration in their professional and private milieu.
Social care management, on the other hand, mainly concentrates on the processing of the disability registration process, the provision of social support measures and the future career planning following injury. Social case management needs to take into account the medical diagnosis, the outcome of treatment and the assessment of the physical and mental status of the patient.
The establishment of a relationship between medical officer and patient based on trust is an important factor with regard to re-integration and improvement of resilience and employability of injured military personnel. In order to implement their concept, the medical services collaborate with the Bundeswehr's mental health services of the Bw and its personnel department with its various responsibilities (personnel management, social services, vocational training). In addition, the medical services also cooperate closely with civilian healthcare service providers in order to ensure that a holistic support structure is in place. The relevant activities can be subsumed in three areas:
- The maintenance of an uninterrupted support and care programme for Bw personnel who have been injured in the line of duty
- Digital data management
- Information management and public relations
The maintenance of an uninterrupted support and care programme for Bundeswehr personnel who have been injured in the line of duty
Rehabilitation commences at the scene at which the injury is sustained. Following competent provision of first aid in the theatre of operations, patients are repatriated and undergoe further in-patient treatment in Bw and/or civilian hospitals until they can be discharged. The Patient Evacuation Coordination Cell (PECC) is responsible for patient tracking from the field medical facility until discharge in the homeland. Spiritual counsellors, military psychologists and superiors begin to provide their services while the patient is still in the theatre of operations, which also includes at this early point in time the provision of support to families. It has been demonstrated that readjustment of family members can be effective. At the commencement of hospital treatment in the homeland, individual case-related rehabilitation teams are formed with the task of planning the course of therapy and rehabilitation measures. These continue to be provided after the return of the patients to their domestic environment by the regional medical institutions and their psychosocial networks. A central coordination and contact centre in the German Armed Foces Federal Personnel Office brings together medical and social care management, provides for the necessary exchange of information and involves superior officers with their final responsibility for the case in the rehabilitation process.
The disability prevention programme of the Bundeswehr Centre for Sports Medicine for personnel injured in the line of duty
As part of the continuous care chain, the Bundeswehr Centre for Sports Medicine in Warendorf manages and provides individualised 'life-long rehabilitation' measures. The centre specialises in interdisciplinary orthopaedic, performance and preventative examination, counselling and treatment. This includes, in addition to performance and functional diagnostics, intensive rehabilitation therapy. Prioritised target groups are members of the Special Forces and top athletes of the Bw, senior military officers and personnel who have developed a physical disability following chronic illness or injury while on duty.
Working closely with the Bw hospital network, the regional healthcare facilities, the Federal Personnel Office of the Bw and the local psychosocial services, the centre provides support with assessments and makes personnel available for the interdisciplinary rehabilitation teams for each individual case. The assessment of the suitability for participation in the centre's own prevention programme and the individual design of each programme is the responsibility of the centre's specialists following the referral of a patient by a medical officer. Assuming that sufficient resources are available, members of the Bw with persistent musculoskeletal or neurological disabilities following non-deployment related accidents, operations or disorders can also participate in the programme if their disability is such that it represents a long term impairment of their functional capacity and risk factors have developed that could result in further restriction of mobility and autonomy with increasing age.
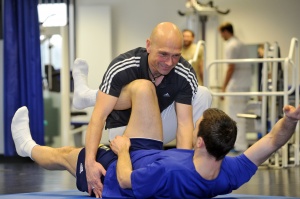
Participation in the programme is voluntary. During an initial interview, patients are instructed in detail of the form, content and aims of the programme and are given the opportunity to decide whether they wish to subsequently participate. Particular emphasis is placed on a comradely and empathic approach. The patients are informed, for example, that if they choose to participate, a team of committed specialists will be assigned to their case who will be designing extensive and individualised measures to positively influence their future life and achieve concrete case-based aims. In order to stress the need for personal commitment and also to avoid the risk that the individual may subsequently feel overwhelmed, patients are also informed that considerable self-discipline, willingness to exercise and determination will be needed if the programme is to be successful. Experience has shown that this combination of highly professional support, personal commitment and self-empowerment represents a particularly effective motivating force for participants. The medical history of patients willing to join the programme is documented, they are given a physical examination and the rehabilitation measures are planned, including the issue of any orthopaedic aids they may need.
The centre's specialists make the final decision with regard to participation and the individual design of the programme. This will include continuous out-patient care, individual intensive rehabilitation treatment and participation in sports therapy courses depending on case.
The programme requires patients to report regularly in accordance with their individual care plan (at least once every 3 months) for out-patient appointments in order to assess their progress in preventive medical terms. During the first examination visit, each patient's performance and functional capacity will be assessed in detail with the aid of procedures such as lactate threshold and isokinetic strength testing, the results of which serve as the basis for further training recommendations and their planning.
Patients with particularly severe musculoskeletal disabilities are first assigned to a 2- to 4-week intensive course of rehabilitation in the Centre of Sports Medicine during which they receive the full spectrum of physiotherapy treatment, which includes individual training and aqua therapy with a personal physio. Such highly intensive and complex therapy concepts designed to extensively restore functionality and mobility and provide for integration are doomed to failure without daily interaction within the team of physician, physiotherapist and patient; in addition, they require a high degree of motivation, self-discipline and stamina on the part of the patient. It is often the case that a physiotherapist who is in constant physical contact with the patient assigned also becomes the emotional conduit through whom the patient attempts to process the fate suffered; to meet this particular challenge physiotherapists require social skills, emotional sensitivity and experience.
Sports therapy as a component of long term disability prevention programmes
The efficacy of sports therapy as a means of achieving the psychological and physical rehabilitation of injured and disabled persons has been scientifically demonstrated. It is far more than just the provision of short term training designed to improve physical capabilities. It is actually an essential prerequisite for long term physical and mental reactivation while it also promotes the implementation and maintenance of a health-orientated lifestyle that will ensure retention of mobility and autonomy of a disabled person even into old age. Assuming that the mental and physical requirements are in place, an interdisciplinary team at the Centre of Sports Medicine will decide on whether sports therapy is appropriate and draw up a performance and resilience capacity profile together with an individual training plan that will be implemented in the form of courses provided by the Bw School of Sport. The courses are provided by the 'Sports therapy after injury in the line of duty' group, members of which include two field officers who usually have experience of active deployment, have completed a 3½ year university course during their officer training and hold a diploma in sports science. This combination of experience of serving abroad and sports science expertise means that they not only have the skills to treat the injured personnel in their care but also understand their problems and what they have been through. They are provided with additional support by a military psychologist with experience of serving in the field who actively takes part in the sports training programme and can thus document the various social interactions between the participants. In addition, the participant's families are also offered spiritual support through the military chaplains’ organisation.
Conclusions
The concept for the care of Bw personnel who have suffered injuries in the line of duty represents a practical implementation of the requirements of the UN Convention on the Rights of Persons with Disabilities and the definition of the bio-psychosocial model for rehabilitation of the WHO. Military personnel who are wounded, injured or mentally traumatised in the line of duty are cared for by the Bw hospital network, specialised civilian health facilities, the regional medical institutions and the local psychosocial services to ensure that they can remain as far as possible within their accustomed social structures and familiar environment. The personal, social and vocational measures required for social case management are centrally coordinated by the German Armed Foces Federal Personnel Office. The Bw Centre of Sports Medicine also offers an extensive interdisciplinary sports medicine-based life-long rehabilitation programme for the prevention of disability in order to provide all those affected with the best possible level of functionality, mobility, autonomy and integration. In addition to continuous cross-disciplinary out-patient care, this includes performance and functional diagnostic measures, specialised intensive in-patient rehabilitation therapy, the planning and management of training and sports therapy courses at the Bw School of Sport. Assuming that sufficient resources are available, patients with severe musculoskeletal disabilities following non-deployment related injuries or disorders can also benefit from the programme. The overall concept is subject to continuing development to make sure that it meets the needs of disabled service personnel. The exchange of experience, knowledge and shared projects with our NATO partners contribute towards the success of this concept for integration and inclusion based on care, comradeship and the use of military structures and skills that can thus serve as a model for corresponding concepts in the civilian sector.
References: ref@mci-forum.com
Date: 12/20/2018
Source: Medical Corps International Forum (1/2015)